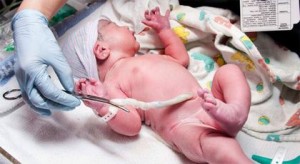
Postpartum care: What to expect after a vaginal delivery
Your newborn may be your top priority — but postpartum care counts, too. From vaginal soreness to urinary problems, here’s what to expect as you recover from a vaginal delivery
Pregnancy changes your body in more ways than you might have guessed, and it doesn’t stop when the baby is born. Here’s what to expect after a vaginal delivery.
Vaginal soreness
If you had an episiotomy or vaginal tear during delivery, the wound might hurt for a few weeks. Extensive tears might take longer to heal. In the meantime, you can help promote healing:
• If sitting is uncomfortable, sit on a pillow or padded ring.
• Use a squeeze bottle to pour warm water over your vulva as you’re urinating. Press a clean pad or washcloth firmly against the wound when you bear down for a bowel movement.
• Cool the wound with an ice pack, or place a chilled witch hazel pad between a sanitary napkin and the wound.
• Take pain relievers or stool softeners as recommended by your health care provider.
While you’re healing, expect the discomfort to slowly improve. Contact your health care provider if the pain intensifies; the wound becomes hot, swollen and painful; or you notice a pus-like discharge.
Vaginal discharge
You’ll have a vaginal discharge (lochia) for a number of weeks after delivery. Expect a bright red, heavy flow of blood for the first few days. The discharge will gradually taper off, becoming watery and changing from pink or brown to yellow or white.
Contact us if:
• You have heavy vaginal bleeding
• The discharge has a foul odor
• You have a fever of 100.4 F (38 C) or higher
Contractions
You might feel contractions, sometimes called afterpains, during the first few days after delivery. These contractions — which often resemble menstrual cramps — help prevent excessive bleeding by compressing the blood vessels in the uterus. These contractions tend to be stronger with successive deliveries. Your health care provider might recommend an over-the-counter pain reliever.
Contact your health care provider if you have a fever or if your abdomen is tender to the touch. These signs and symptoms could indicate a uterine infection.
Urination problems
Swelling or bruising of the tissues surrounding the bladder and urethra can lead to difficulty urinating. Fearing the sting of urine on the tender perineal area can have the same effect. Difficulty urinating usually resolves on its own. In the meantime, it might help to pour water across your vulva while you’re sitting on the toilet.
Contact your health care provider if you have any signs or symptoms of a urinary tract infection. For example:
• A strong, persistent urge to urinate
• A burning sensation when urinating
• Passing frequent, small amounts of urine
Pregnancy and birth stretch the connective tissue at the base of the bladder and can cause nerve and muscle damage to the bladder or urethra. You might leak urine when you cough, strain or laugh. Fortunately, this problem usually improves with time. In the meantime, wear sanitary pads and do Kegel exercises to help tone your pelvic floor muscles.
To do Kegels, tighten your pelvic muscles as if you’re stopping your stream of urine. Try it for five seconds at a time, four or five times in a row. Work up to keeping the muscles contracted for 10 seconds at a time, relaxing for 10 seconds between contractions. Aim for at least three sets of 10 repetitions a day.
Hemorrhoids and bowel movements
If you notice pain during bowel movements and feel swelling near your anus, you might have hemorrhoids — stretched and swollen veins in the anus or lower rectum. To ease any discomfort while the hemorrhoids heal, soak in a warm tub and apply chilled witch hazel pads to the affected area. Your health care provider might recommend a topical hemorrhoid medication as well.
If you find yourself avoiding bowel movements out of fear of hurting your perineum or aggravating the pain of hemorrhoids or your episiotomy wound, take steps to keep your stools soft and regular. Eat foods high in fiber — including fruits, vegetables and whole grains — and drink plenty of water. Ask your health care provider about a stool softener or an osmotic laxative, if needed.
Another potential problem for new moms after a vaginal delivery is the inability to control bowel movements (fecal incontinence). Frequent Kegel exercises can help with mild fecal leakage. If you have persistent trouble controlling bowel movements, consult your health care provider
Sore breasts and leaking milk
Several days after delivery, your breasts might become firm, swollen and tender (engorgement). To ease discomfort, nurse, use a breast pump, apply warm washcloths or take a warm shower to express milk. Between feedings, place cold washcloths or ice packs on your breasts. Over-the-counter pain relievers might help, too.
If you’re not breast-feeding, wear a firm, supportive bra, such as a sports bra, to help stop milk production. Don’t pump or rub your breasts, which will cause your breasts to produce more milk. If feedings are painful, ask a lactation consultant for help.
If your breasts leak between feedings, wear nursing pads inside your bra to help keep your shirt dry. Change pads after each feeding and whenever they get wet.
If you’re not breast-feeding your baby, wear a firm, supportive bra to help stop milk production. Don’t pump your breasts or express the milk, which will cause your breasts to produce more milk.
Hair loss and skin changes
During pregnancy, elevated hormone levels put normal hair loss on hold. The result is often an extra-lush head of hair — but now it’s payback time. After delivery, your body sheds the excess hair all at once. Hair loss typically stops within six months.
Stretch marks won’t disappear after delivery, but eventually they’ll fade from reddish purple to silver or white. Expect any skin that darkened during pregnancy — such as the line down your abdomen (lineanigra) — to slowly fade as well.
The postpartum checkup
About six weeks after delivery, your health care provider will check your vagina, cervix and uterus to make sure you’re healing well. He or she might do a breast exam and check your weight and blood pressure, too. This is a great time to talk about resuming sexual activity, birth control, breast-feeding and how you’re adjusting to life with a new baby. You might also ask about Kegel exercises to help tone your pelvic floor muscles.
Above all, share any concerns you might have about your physical or emotional health. Chances are, what you’re feeling is entirely normal. Look to your health care provider for assurance as you enter this new phase of life.
You have a brand-new baby — and you also just had surgery. Whether you knew you would get a c-section or not, dealing with both at the same time can be rough. Here’s what you’re in for, and ways to ease and speed your recovery.
Wait the right amount of time to move around
You won’t be pacing the room rocking your newborn right after delivery, but you should be able to get out of bed and walk around within a day. Why the wait? First, the numbing medications have to wear off (our guess is you actually want to be able to feel your legs). And some women, especially those who had a long labor before they had a c-section (if that’s you, we’re so sorry), need extra time to regain their energy. Once the catheter is removed (it emptied your bladder so it wouldn’t be damaged during delivery), you’ll be able to get out of bed. And you should (at least a little bit); moving around will help you recover.
Being active allows normal body functions to get back to their routine, as well as decreasing the chance of a postoperative complication.For example, being sedentary can cause the bowels to move more slowly, leading to constipation. It can also be a serious risk factor for forming a blood clot in the leg or acquiring a postoperative pneumonia.
Of course, you’re not going to get up and go for a sprint anytime soon — it’s important to take the time to let your body heal before you jump back into exercise — but gradually increase the amount of activity you do around two weeks postpartum. “That can mean walking longer distances and becoming more active.Increase the intensity around six weeks postpartum.By that time, you should have a follow-up appointment with your OB, who will likely clear you for more intense exercise (and sex too, not that you’ll be interested!).
Just say yes to the pain meds
Expect the c-section incision to hurt for a while. Medications delivered through the epidural ease pain immediately after delivery. After you’re done with those, you’ll be given oral anti-inflammatory medication. These meds don’t interfere with breastfeeding,
Every new mom gets cramping after delivery — that’s the uterus’s way of shrinking to its original size, and it will probably clear up within two weeks post-birth — and having that incision will make it more intense for you. Also know that breastfeeding can trigger those cramps and make the pain even worse. That’s all the more reason to keep taking your meds. Talk to your doctor or a lactation consultant if you’re having severe pain or other problems breastfeeding.
Expect bleeding
Even though you didn’t deliver vaginally, you will have postpartum vaginal bleeding. The blood comes from the area of the uterus that used to be attached to the placenta. “The bleeding is part of the healing process in your uterus
Care for your incision
In the shower, let soapy water drip on the wound (don’t scrub). Pat it dry. If your skin folds over the incision, put a cloth pad on it to keep it from getting sweaty. Within a week, your wound will be mostly healed. But look out for issues: If you develop a fever or if the skin surrounding the incision turns red, it starts oozing green or pus-colored liquid, or it becomes hard or painful, call your doctor. These could be signs of infection.
And don’t worry just yet about scarring — yes, you’ll have one and there’s no way of knowing exactly how it will look once it heals. “Any incision is going to leave a scar. “How much of a scar is determined by your own genetics.” Once your wound has healed, about six weeks after delivery, you can use scar-reducing ointments to help with the appearance. The color will likely fade, but it will be there. For most c-section mamas, the scar is horizontal and falls under the bathing suit line, so you’ll probably be able to wear a two-piece someday (yay!).
Take good care of yourself
Sure, you’re a new mom with a round-the-clock new responsibility, but it’s important for both you and baby that you recover quickly. Help speed recovery by eating nutritious foods, getting as much rest as you can and exercising once you get the go-ahead from your doctor. Don’t be afraid to ask for a little help so you can get some extra sleep, take a long shower or eat a full meal.